- An endocrine gland situated at the root of the neck, one on either side of the trachea.
- Bi-lobed, connected to each other by an isthmus.
- Weight is about 20-40gm, 4 to 4.8 x 1 to 1.8 x 0.8 to 1.6 cm in size, in adults.
- Larger in females as compared to males.
- Changes occur in structure and function in different stages of sexual cycles in females.
- Pregnancy and lactation increases its function slightly.
- In menopause, its function declines.
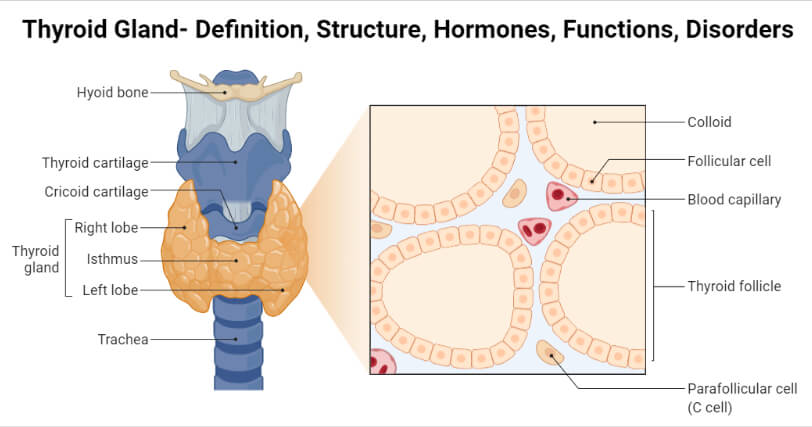
Image source: biologynotes
Histology of Thyroid gland
- Contains large number of closed follicles lined with cuboidal epithelial cells.
- So the cells are called follicular cells.
- Thyroglobulin, a colloidal substance, is secreted by these follicular cells.
- This substance fills the follicular cavity.
- Tetra-iodothyronine (T4 or thyroxine) and tri-iodothyronine (T3) are also secreted by these cells.
- Parafollicular cells present in between follicles which secretes calcitonin.
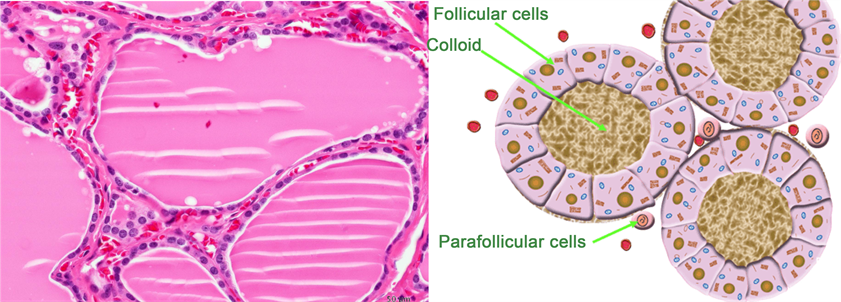
Image source: scientificresearch
Hormones of Thyroid gland
- T4, T3 and calcitonin are the main hormones secreted.
- T4 also called thyroxine forms about 90% of secretion.
- T3 forms only 9-10% of total secretion.
- T4 and T3 are derivatives of amino-acids tyrosine which contains iodine.
- T3 has four times more potency than T4 though T3 acts for shorter period than T4.
- T4 has more affinity and binds strongly with plasma proteins so released slowly and acts longer.
- T3 has less affinity with plasma proteins and binds loosely, so released quickly and acts shorter.
- Therefore, T4 acts slowly on the target cells than T3.
- T4 has half-life of 7 days which is longer than in T3 i.e. T3 has between 10 and 24 hours.
- T4 is secreted more i.e., 80-90 μgm/day whereas T3 is 4-5 μgm/day.
- Reverse T3 is secreted only about 1-2 μgm/day.
- Plasma level of T4 is more i.e., 8 μgm/dl whereas T3 is 0.12 μgm/dl.
- In muscles, liver and kidney, thyroid hormones generally degrades.
Thyroid Hormones Synthesis
- In thyroglobulin present in follicular cavity, thyroid hormones synthesis occurs.
- Iodine and tyrosine from diet absorbed from GI tract, are essential materials for its formation.
- Iodine is converted to iodide.
- 1mg of iodine per week or about 50 mg/year iodine is required.
- Salt is iodized with one part of sodium iodide to every 100,000 parts of sodium chloride to prevent iodine deficiency.
- In five stages, synthesis of these hormones occurs. They are:
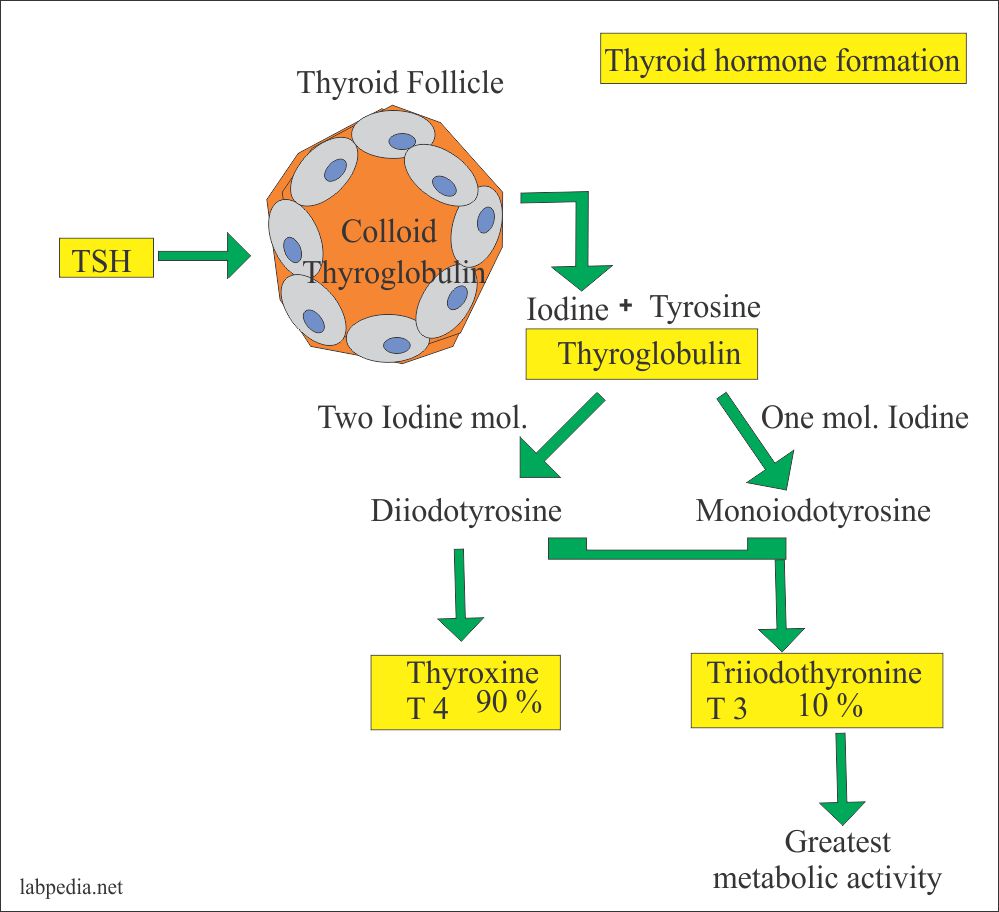
Image source: labpedia
a) Thyroglobulin synthesis
- Thyroglobulin is secreted by ER and golgi apparatus of the follicular cells continuously.
- Each thyroglobulin molecule contains 140 molecules of amino acid tyrosine.
- Thyroglobulin is stored in the follicle after synthesis which is a large glycoprotein.
b) Iodide trapping
- From blood, iodide is carried to follicular cell against electrochemical gradient.
- This process is known as iodide trapping.
- Sodium-iodine symport pump helps to transport iodide along with sodium.
- This pump is also called iodide pump.
- Iodide is 30 times more concentrated in thyroid than in blood.
- Hyperactivity of thyroid gland increases iodide concentration by more than 200 times.
c) Iodide oxidation
- Iodine is required to combine with tyrosine to form thyroid hormones.
- So iodide is oxidized to form iodine which is the elemental form.
- This oxidation process occurs in follicular cells.
- It occurs in presence of thyroid peroxidase.
- This enzyme absence or inactivity stops thyroid hormones formation.
d) Transport of iodine to follicular cavity
- Iodine is transported to follicular cavity later on by an iodide-chloride pump.
- This pump is also called pendrin.
e) Iodination of Tyrosine
- Iodination means combination of iodine with tyrosine.
- It occurs in thyroglobulin.
- Iodine is first carried to follicular cells into the follicular cavity.
- In this cavity, iodine binds with thyroglobulin.
- This process is called organification of thyroglobulin.
- Tyrosine present in the thyroglobulin then combines with iodine.
- Iodinase enzyme secreted by follicular cells accelerates this iodination process.
- This process occurs in different stages.
- Firstly, monoiodotyrosine (MIT) is formed which later converted to diiodotyrosine.
- MIT and DIT are also known as iodotyrosine residues.
f) Coupling reactions
- The above residues get coupled with each other.
- Coupling occurs in different configurations to give different thyroid hormones.
- Coupling reactions includes following steps:
i) One molecule MIT and one molecule of DIT forms tri-iodothyronine(T3).
ii) Sometime the above reaction yields another form of T3 called reverse T3 or rT3.
iii) This form of T3 is 1% of thyroid output.
iv) Two molecules of DIT form tetra-iodothyronine which is also called thyroxine.
Storage of thyroid Hormones
- Remains in the form of vesicles within thyroglobulin.
- Stored here in this form for longer period.
- 5-6 molecules of thyroxine are present in each thyroglobulin molecule.
- In average, 1 triiodothyronine molecule is present for every 10 molecules of thyroxine.
- In combination form, the thyroid hormones can be stored for long time i.e., for several months.
- This is the only endocrine gland for storing hormones for about 4 months.
- Signs and symptoms of deficiency to these hormones, do not appear for about 4 months though synthesis of hormones stops.
References:
i) https://www.ncbi.nlm.nih.gov/books/NBK551659/
ii) https://www.uptodate.com/contents/image?imageKey=ENDO%2F76931
iii) https://www.biosciencenotes.com/thyroid-gland-and-thyroid-hormones/
iv) https://www.simplepharmanotes.com/2021/08/thyroid-gland.html

